Over a thousand babies born in the UK each year suffer brain injuries during birth, often resulting in death or lifelong disability. A team of researchers at Oxford University is developing a big data-powered decision-support system to help midwives cut the risk of these injuries.

Contractions during childbirth can cause brain injuries in the baby, explained Antoniya Georgieva, associate professor and group lead at the Oxford Labour Monitoring unit at the Nuffield Department of Women’s & Reproductive Health, at a conference this month.
This affects 1,200 babies a year, she said during a Westminster eForum event, and can result in death or lifelong disability. “Contractions during labour squeeze the placenta, the cord [and] the baby, and some small proportion of babies will suffocate during childbirth, which is clearly a very tragic event for all involved,” Georgieva explained.
“Over half of these incidents are preventable with better monitoring and care during childbirth-friendly clinical interventions,” she added.
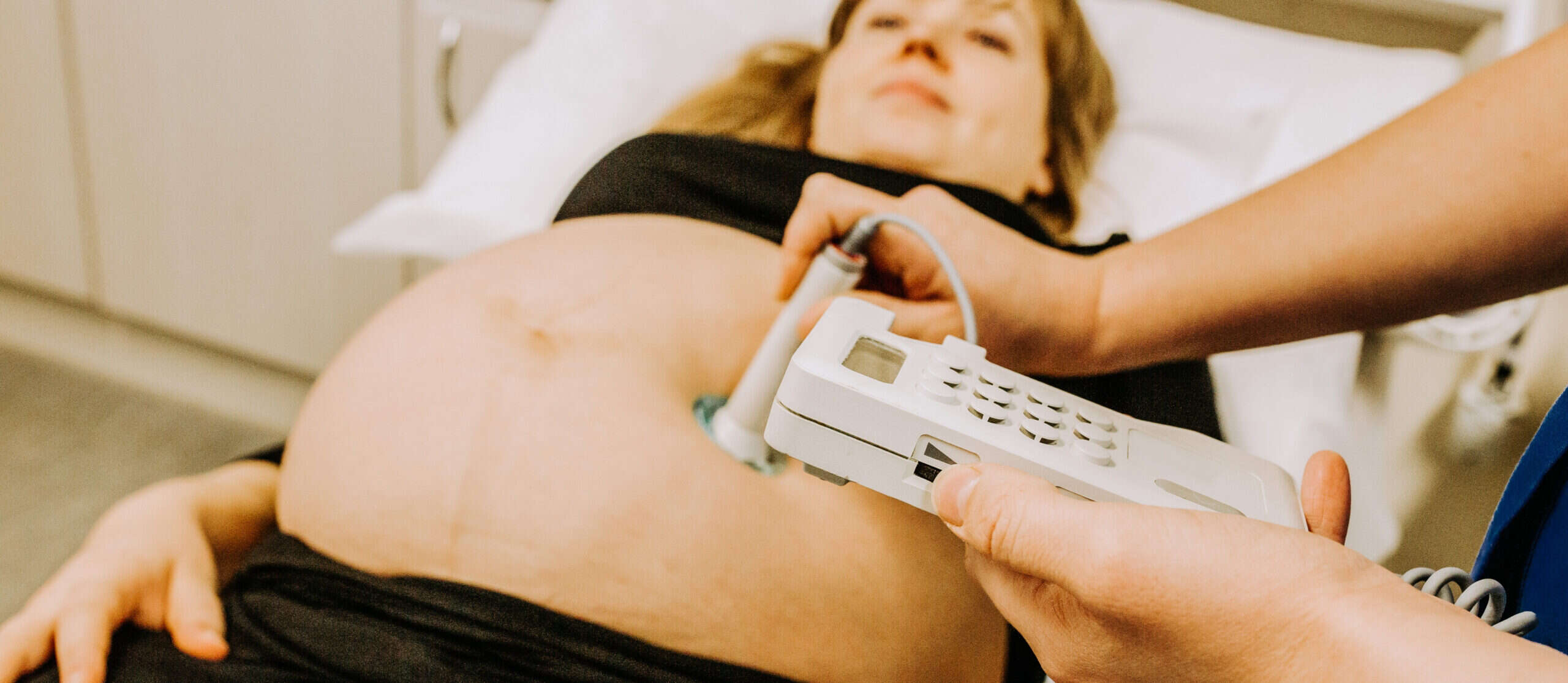
At-risk mothers and their babies are monitored during labour using a device called a cardiotocograph, which is strapped onto the abdomen and measures the foetal heart rate and contraction of the uterus. Midwives and doctors use the paper readout from these devices to determine whether an intervention, such as a C-section, is needed.
Cardiotocographs are the only way to monitor the baby during labour, explains Georgieva, so the data must be analysed effectively. “We don’t have blood pressure for the baby, we don’t have blood flow to the brain for the baby, and these things change dynamically during labour so it’s a very big challenge.”
Practitioners’ interpretation of cardiotocograph data is known to be highly variable, however, Georgieva says. And the limitations of that data when used in isolation are “very well-documented,” she says.
Improving the analysis of cardiotocograph data to prevent brain injuries during labour is the motivation behind the work of Georgieva and her team. “That’s why we are doing our research at Oxford.”
Big data methods for assessing brain injury risk
Georgieva’s team is developing a system, named OxSys, that predicts the risk of brain injury during labour. The system draws on the records of more than 100,000 deliveries collected by the department, which includes data about the mother and baby’s health.
Cardiotocographic data from these deliveries has been integrated with historic health records, thanks to the “meticulous” work of departmental colleague Professor Chris Redman, Georgieva told Tech Monitor, “and the excellent integration between the University and the NHS at Oxford, which allows us to be at the forefront of many clinical research fields”.
Combining these datasets allows Georgieva and her team to understand cardiotocograph data in context, she explains. “We need a lot of other information around the [cardiotocograph] such as maternal comorbidities, pregnancy and labour complications, the age of the baby and the mother.”
The team is now evaluating the best way to analyse this historic data so that real-time cardiotocograph data can be used to assess the risk of injury during delivery. An early version of OxSys used a simple machine learning algorithm to model the data. This algorithm “compares [to] or slightly outperforms clinical practice,” Georgieva told Tech Monitor.
Now, they are examining more advanced analytical methods. These include convolutional neural networks and other deep learning methods, Georgieva continues, which have had “promising results”, so far, and which the team is working to improve on.
Another approach is statistical prognostic modelling, which uses conventional statistical techniques to assess healthcare risk. This approach, which allows the team to combine clinical risk factors with cardiotocograph data “in a very clinically meaningful way”, is also performing well in early experiments, Georgieva told Tech Monitor. Her personal view is that this approach will be the first to reach clinical trials.
Decision support for midwives
To help midwives use OxSys in practice, the team has developed a tablet app. Real-time data from the cardiotocograph is analysed, in combination with mother and baby’s clinical records, to provide a live risk estimate. The healthcare practitioner can use this to determine whether a C-section or other intervention is required.
Georgieva stresses that the OxSys tech is a decision-support tool, not a replacement for human workers. “I think it is really important to say that there is no tech solution that would come and replace midwives,” she explains. Instead, its purpose is to save them from performing “mental arithmetic gymnastics” when deciding whether an intervention is necessary.
For now, Georgieva and her team are focused on developing OxSys to provide even more accurate predictions. This includes adding 40,000 more delivery records into the analysis.
They are also seeking ways to scale its testing and use, although Georgieva is hesitant to commercialise the application. She fears that this would mean the team’s research becomes proprietary and that OxSys would become too expensive. “When money is driving [them], products cost a lot more and there’s no support afterwards for the people using them.”






