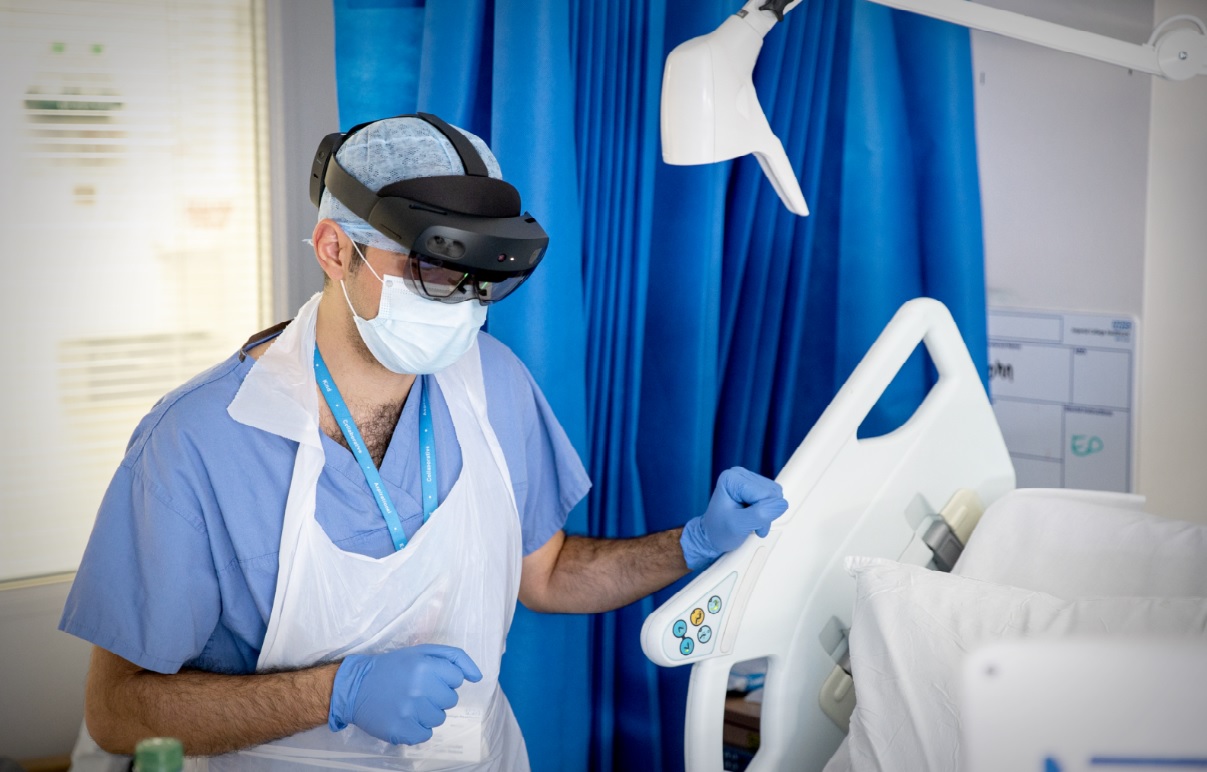
A London NHS trust trialling the use of augmented reality (AR) headsets says it could slash the amount of personal protective equipment (PPE) needed, and reduce the number of medical staff exposed to highly contagious patients.
The Imperial College Healthcare Trust is using HoloLens headsets to let medical staff “remotely join” consulting clinicians who are delivering oxygen therapy in high-risk patient areas, a new academic paper reveals.
“Pre-deployment practice was two or more staff donning PPE for ward rounds and to review deteriorating patients. Following deployment of HoloLens2, one doctor would conduct the ward round wearing the device and other team members would remain protected in the ‘clean’ area whilst participating virtually in care delivery”, the non-peer reviewed paper notes.
NHS AR Headset Trials: Why Was the Trial Conducted?
The need for such technology has arguably intensified, given PPE supply chain problems and the aerosol generating procedures carried out during oxygen therapy, which expose healthcare givers to a significant viral load.
The trust — which includes St Mary’s, Charing Cross, and Hammersmith Hospitals — noted: “Staff delivering such interventions require PPE and are exposed to a significant viral load resulting in sick days and even death.”
 NHS AR Headsets Trials
NHS AR Headsets Trials
Using HoloLens, one consultant can do the rounds in a Coronavirus ward and share processes with other doctors via Microsoft Teams, the report — by five Imperial College and NHS Trust authors — noted in a May 24 pre-print.
Headset use also resulted in reduced time in high-risk zones, but the difference was “not statistically significant”, the authors admit.
They claimed, however, that use of the AR headset nearly halved PPE use, “did not impair communication, medical staff availability or end of life care”.
HoloLens headsets, built by Microsoft, are powered by a Quallcomm Snapdragon 850 chip and feature Bluetooth 5.0, an 8MP stills camera and 1080p video. They retail at approximately £3,000.
HoloLens maker Microsoft provided devices and technical support, but did not participate in the write up or review of the manuscript.

Consultant Surgeon at Imperial College Healthcare James Kinross explained the success of the tool so far in a Microsoft release:
“In March, we had a hospital full of Covid-19 patients. Doctors, nurses and allied healthcare professionals providing ward care had a high risk of exposure to the virus and many became ill. Protecting staff was a major motivating factor for this work, but so was protecting patients. If our staff are ill they can transmit disease and they are unable to provide expert medical care to those who needed it most.
“We needed an innovative solution. I’ve used HoloLens before in surgery and we quickly realised it had a unique role to play because we could take advantage of its hands-free telemedicine capabilities. Most importantly, it could be used while wearing PPE. It solved a major problem for us during a crisis, by allowing us to keep treating very ill patients while limiting our exposure to a deadly virus. Not only that, it reduced our PPE consumption and significantly improved the efficiency of our ward rounds”.
The paper’s authors acknowledged that HoloLens use can “complicate critical non-verbal areas of communication like eye contact, and patient experience must be a measure of future implementation.”
“Finally, lack of randomization and lack of control for patient numbers introduces further potential bias. During implementation, we needed to address concerns about data security, patient safety and cost.”

 NHS AR Headsets Trials
NHS AR Headsets Trials




